Introduction
Imagine waking up after eight solid hours of sleep, tracking sleep stages on a wearable, hitting your macros, and still feeling like someone pulled the battery out of your body. Meetings blur together, workouts feel twice as hard, and even fun plans start to sound like work. At that point the real question is not “Why am I tired?” but “Is this normal fatigue vs burnout starting to take over?”
Fatigue is part of being human. Burnout is different. It is a state where exhaustion seeps into how a person thinks, feels, and sees themself. Between those two sits overwhelm, where the to‑do list expands faster than the energy to handle it. These three states share symptoms, which is why so many high performers misread deep burnout as “just stress” and try to fix it with more coffee, another productivity hack, or one more hard training block.
For people serious about performance and longevity, confusing fatigue vs burnout has a cost. Rest days and caffeine can fix basic fatigue. Burnout, on the other hand, changes brain circuits, drains cellular energy, and often needs months of structured recovery. This guide walks through the full spectrum: how to tell what is going on, what happens in the brain and mitochondria under chronic stress, and how to fight burnout—and then how to fix burnout—with both lifestyle shifts and advanced tools.
Along the way, you will see where cellular energy and NAD+ fit in, and how physician‑formulated nasal sprays from Synchronicity Health aim at the root of persistent exhaustion rather than just covering it up. By the end, you will have a clear map to spot warning signs early, choose the right level of intervention, and build a system that supports high output without burning out the hardware.
“You can’t pour from an empty cup. Take care of yourself first.” — Popular saying
Key Takeaways
-
Fatigue vs burnout is mostly about depth and reversibility. Fatigue is a temporary state with a clear cause that tends to resolve with rest, while burnout is a chronic collapse of energy, motivation, and sense of self that keeps going even after breaks and vacations. Overwhelm sits in the middle as a phase of “too much at once” that can slide either way.
-
Burnout is not just a mood problem. Brain imaging studies show less gray matter in areas that manage focus and emotional control, plus a hyperactive amygdala that holds the nervous system in high alert. This is why someone can feel “wired but tired,” anxious, and unable to calm down even when nothing urgent is happening.
-
The most reliable quick test is how energy responds to rest. When a long weekend, lighter training week, and better sleep restore drive, the problem is mostly fatigue. When dread, numbness, and exhaustion snap back as soon as normal life resumes, burnout is far more likely and needs a different approach.
-
The most effective way to fight burnout combines foundations like sleep, nutrition, movement, boundaries, and social support with deeper tools such as therapy, stress skills, and, when needed, cellular support. NAD+ support, metabolic tuning, and adaptogens help refill the “battery” that chronic stress empties.
-
Professional help is needed when exhaustion and hopelessness persist despite lifestyle changes, work or home functioning collapses, or substances become a main coping tool. Cellular energy optimization from brands like Synchronicity Health can speed repair, but it works best alongside medical, psychological, and behavioral care.
Understanding Fatigue: The Body's Natural Response To Overexertion
Fatigue is the body’s feedback system. It is how cells, muscles, and the brain signal that current demands are higher than the available energy or recovery. In simple fatigue, that signal is temporary and linked to something obvious such as a late night, back‑to‑back meetings, travel, a hard training cycle, or fighting off a virus.
For most people, this kind of tiredness fades when the stressor passes and recovery time appears. Sleep improves, soreness eases, and mental sharpness returns. Fatigue itself is not the enemy; ignoring it is. High performers often treat tiredness as a mindset problem instead of a biological limit and try to outwork the signal. Over time, that pattern pushes the system from short‑term fatigue toward chronic depletion.
Where fatigue becomes risky is when it drags on for weeks, does not change much with extra sleep, and starts mixing with apathy or dread. At that point, it becomes harder to tell if this is still basic tiredness or the early slide toward burnout. Understanding which type of fatigue is present is the first step in choosing the right fix.
The Three Primary Types Of Fatigue
Fatigue is not one single feeling. It shows up in the body, in thinking, and in emotional life, and each type has different triggers and recovery paths. Most people have a dominant pattern, but all three can combine during stressful seasons or illness.
-
Physical Fatigue
Physical fatigue sits in muscles, joints, and overall body heaviness. It often appears after:-
Long shifts on the feet
-
Intense training blocks
-
Poor sleep
-
Dehydration or under‑eating
A person with physical fatigue may notice that climbing stairs feels harder, weights feel heavier, or heart rate runs higher than usual for the same workload. When physical fatigue is the main issue, a few nights of high‑quality sleep, better hydration, and deloading workouts usually reverse it within days.
-
-
Cognitive Fatigue
Cognitive fatigue lives in the brain. It feels like fog or a dimmer switch on mental sharpness, and it often comes from long periods of deep work, constant multitasking, or screen overload. Sleep loss, jet lag, and stress magnify it. At the cellular level, the brain is burning through ATP and NAD+ to keep up, and when those resources run low, focus, memory, and reaction time slip. Dealing with cognitive fatigue means more than just motivation; it often requires real breaks from screens, protected focus blocks, and support for cellular energy. -
Emotional Or Psychological Fatigue
Emotional fatigue shows up as feeling done with everything, even activities that used to be energizing. It often follows months or years of caregiving, ongoing conflict, grief, or high‑empathy work such as healthcare or counseling. People in this state may still sleep but wake feeling empty, unmotivated, or unable to care the way they once did. This pattern is the most likely to blend into burnout if nothing changes, because it touches the systems that control meaning, connection, and purpose.
The Cellular Energy Crisis: Why Your Mitochondria Matter
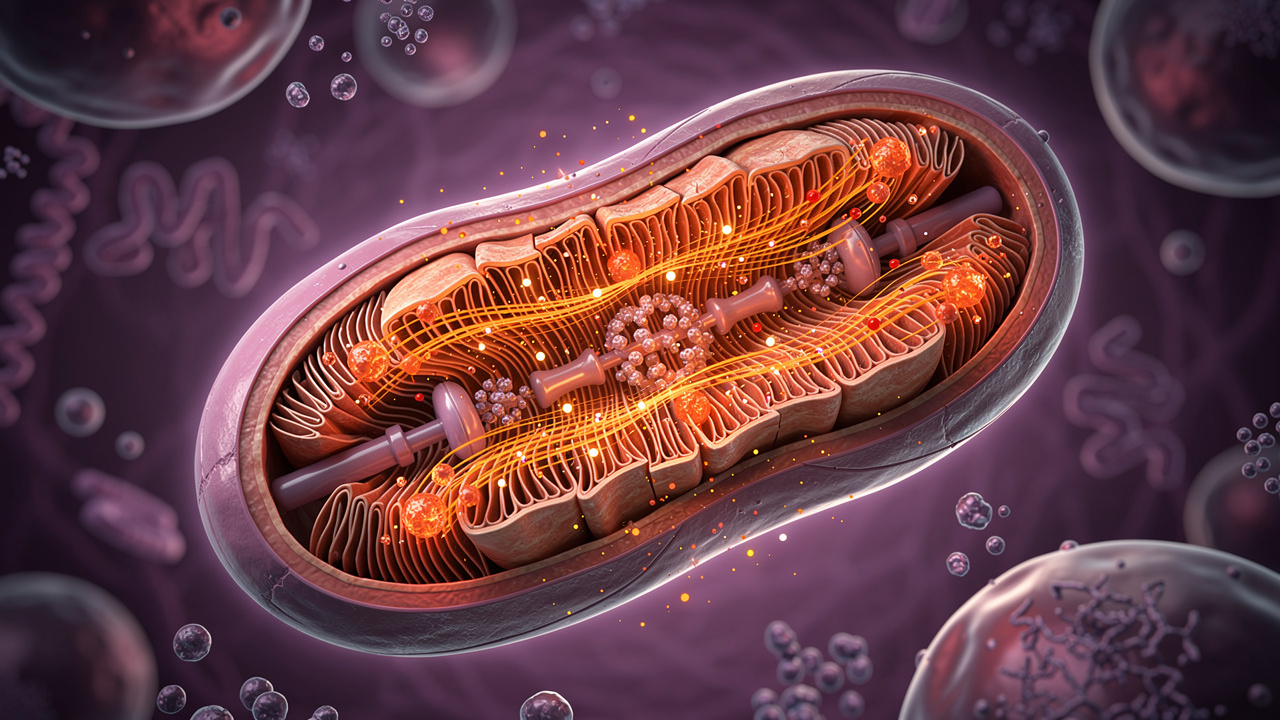
Under all three kinds of fatigue sits the same basic engine: **mitochondria**. These tiny structures inside cells take fuel from food and oxygen from the air and turn them into **ATP**, the energy currency cells use for everything from muscle contraction to firing neurons. When mitochondria run well, people feel steady energy. When they struggle, the first signs are often fatigue, brain fog, and slow recovery. **NAD+ (nicotinamide adenine dinucleotide)** is a key partner in this energy process. It shuttles electrons inside mitochondria so ATP can form. By midlife, average NAD+ levels have dropped have dropped by roughly half compared with youth, and chronic stress, poor sleep, and heavy training can drain it further. When NAD+ runs low, mitochondria cannot keep up, DNA repair slows, and both physical and cognitive fatigue become far more common. This is where the difference between stimulant‑based energy and cellular energy matters:
-
Stimulants like caffeine block adenosine so a person feels less sleepy, but they do not refill ATP or NAD+. It is like turning up the volume on an empty speaker.
-
Cellular energy support focuses on refilling that ATP and NAD+ pool so cells can truly work better, not just harder.
**Synchronicity Health** focuses on that level by using physician‑formulated **NAD+ nasal sprays** and **NMN** products that aim to deliver NAD+ support with high bioavailability. For someone stuck in a pattern of chronic fatigue, rebuilding mitochondrial capacity can be the missing piece that makes lifestyle changes start to work again.
Defining Burnout: When Exhaustion Becomes A Crisis Of Self

**Burnout** is more than being very tired. It is a state of emotional, mental, and physical collapse that comes from long‑term, unmanaged stress. The World Health Organization lists it as an occupational phenomenon, but real life shows it just as often in parents, caregivers, founders, and anyone carrying heavy responsibility with limited recovery.
“Burn‑out is a syndrome conceptualized as resulting from chronic workplace stress that has not been successfully managed.” — World Health Organization
The key feature that separates burnout from simple fatigue is that it does not fade with normal rest. A person can take a week off and still return feeling dread, emptiness, and resentment toward the same tasks. Sleep may be longer but not refreshing. Things that once felt meaningful start to feel pointless, and even fun plans can feel like pressure.
Researchers and clinicians often describe burnout as a crisis of identity and purpose. Under chronic stress, the brain’s stress circuits stay locked on, while areas that handle focus, emotional balance, and motivation start to go offline. People describe feeling like a hollowed‑out version of themselves, going through the motions with no real engagement. That deeper shift in outlook is what makes burnout different from “just being tired” and why checking the right box on the fatigue vs burnout question matters for recovery.
The Three Core Dimensions Of Burnout
The Costs of Caring: Prevalence and Associated Factors of Burnout, Compassion Fatigue, and Compassion research shows that burnout tends to show up in a specific pattern across different populations. Understanding these three pillars makes it easier to recognize the syndrome early and take it seriously instead of dismissing it as a rough patch.
-
Exhaustion
This is not just needing a weekend to catch up. It is a deep sense of being empty, emotionally and physically, that stays even after extra sleep or time off. People describe waking up tired, feeling drained halfway through the day, and having nothing left for family or hobbies. Immune function often suffers, leading to frequent colds, and sleep patterns can swing between insomnia and oversleeping. -
Cynicism Or Detachment (Depersonalization)
Here, the brain uses emotional distance as a coping move. Work that once felt important becomes irritating. Patients, clients, or coworkers can feel like problems instead of people. Friends and family may notice sarcasm, irritability, or a checked‑out vibe replacing warmth and interest. At first this distance can feel protective, but over time it erodes relationships and makes isolation worse. -
Reduced Efficacy
This is the painful sense that performance is slipping and nothing done makes a difference. Someone in this state may still be working long hours but feel constantly behind, making more mistakes, or stuck in loops of indecision. Creativity drops, problem‑solving feels harder, and confidence erodes. That loss of belief in one’s own effectiveness feeds more stress, which deepens exhaustion and cynicism in a tight feedback loop.
“Burnout is not a problem of people but of the places where they work.” — Christina Maslach, PhD
Comprehensive Symptom Recognition Checklist
Burnout touches the body, emotions, and behavior at the same time. A single symptom does not define it, but a pattern across several areas, lasting for weeks or months, is a strong warning sign. The table below can help with self‑assessment.
|
Category |
Common Symptoms |
How It Often Feels |
|---|---|---|
|
Physical |
Constant tiredness, headaches, muscle tension, frequent illness, gut discomfort, big changes in sleep or appetite |
The body feels heavy and worn out, with nagging aches and a sense of running on fumes even on “easy” days. |
|
Emotional |
Irritability, sadness, numbness, hopelessness, loss of motivation, feeling detached or alone |
Moods swing between flat and overwhelmed, with a loss of joy in things that once mattered and a sense of being trapped. |
|
Behavioral |
Procrastination, missed deadlines, social withdrawal, using food, alcohol, nicotine, or drugs to cope, snapping at others |
Daily tasks pile up, calls and messages go unanswered, and coping leans more on escape than on solving problems. |
Experiencing a few of these now and then is normal. When several symptoms from all three columns show up together for an extended stretch, it is a strong sign that burnout may be developing or already present. At that point, rest alone is rarely enough; a deeper reset is needed.
The Critical Distinctions: Fatigue Vs. Burnout Vs. Overwhelm
A comparison of the course of burnout and prolonged fatigue in research shows that fatigue, overwhelm, and burnout sit on a spectrum of stress and depletion with distinct trajectories. They share features, which is why even doctors and therapists sometimes blur them together. For anyone focused on performance and longevity, though, getting this right matters, because each state calls for a different plan.
-
At one end, simple fatigue is a normal response to high effort. It is unpleasant but short‑lived and tends to respond well to sleep, food, hydration, and a lighter schedule.
-
Overwhelm shows up when demands balloon faster than resources. The inbox fills faster than it empties, the calendar has no white space, and everything feels urgent.
-
Burnout is the far end, where the system has been overloaded for so long that energy, motivation, and meaning collapse.
Thinking of the spectrum as fatigue → overwhelm → burnout helps. A person can move back and forth on it over time. The goal of this section is to show how to tell which zone someone is in so that strategies for how to fight burnout or how to fix burnout are used at the right time and intensity.
Duration And Reversibility: The Rest Test
One of the simplest ways to separate fatigue from burnout is to watch what happens after real rest—not a single early night, but a few days with lighter demands, better sleep, and less stimulation.
-
With fatigue, real rest tends to work. After a quiet weekend, a deload week in the gym, or a short vacation, energy comes back, mood improves, and tasks feel manageable again. The body and brain needed time and nutrients, and once they got both, they shifted back toward baseline within a few days to a week or two.
-
With burnout, rest feels good in the moment but does not change the baseline. People in burnout often describe returning from vacation feeling okay for a day or two, then noticing dread, brain fog, or irritability flood back as soon as messages and tasks restart. Full recovery in these cases often takes three to six months of steady changes, not a single break.
A simple way to frame this is as a decision path in words:
-
If more rest plus lighter demands lead to steady improvement in energy and motivation, the issue is more likely fatigue or early overwhelm.
-
If enough rest has already happened and energy, outlook, and performance still feel stuck or worse, burnout should be on the table and deserves attention.
Emotional And Psychological Impact: Tired Vs. Defeated
The emotional flavor of fatigue vs burnout is very different once a person knows what to look for. Both can bring irritability, low patience, and a shorter fuse, but the deeper layers do not match.
-
In simple fatigue, the core outlook on life tends to stay intact. A tired person may snap more easily or feel less patient, but they can still imagine feeling good after a few nights of sleep or a slow weekend. Projects, relationships, and goals still feel meaningful; they just feel temporarily hard to serve.
-
In burnout, emotions often flatten or swing between numbness and raw distress. People describe feeling empty, hopeless, or disconnected from their own life. Activities that used to feel rewarding become joyless. This is less “I am tired of this week” and more “I do not see the point of any of this.” That inability to picture a better state in the near future is a core sign of burnout.
-
Overwhelm sits in between. It brings a high level of stress, racing thoughts, and anxiety, but the person still cares deeply about outcomes. They want to do well; they just feel buried. When overwhelm goes on for too long without relief, the emotional system may swing into burnout’s numbness as a kind of shutdown mode.
Impact On Motivation And Functioning
Energy, motivation, and performance all shift in different ways across fatigue, overwhelm, and burnout. Looking at daily functioning can make the distinctions stand out more clearly.
-
In fatigue, motivation is still present, but the body and brain struggle to meet it. Tasks take longer, and workouts may feel sluggish, but the person pushes through because the work still feels worth it. Once rest happens, productivity and engagement usually rebound.
-
In burnout, motivation itself crumples. People often describe “going through the motions,” doing the bare minimum to avoid disaster but feeling detached from outcomes. Cynicism makes it hard to care about results, and the sense of inefficacy turns effort into something that feels pointless. That mix leads to missed deadlines, poor performance, and more self‑criticism, which deepens burnout.
-
Overwhelm often looks like frantic engagement. There is a lot of motion, multitasking, and mental load, but effectiveness drops because attention is scattered. In a simple comparison:
-
Fatigue means being slower but steady.
-
Overwhelm looks frantic yet disorganized.
-
Burnout feels frozen or checked out.
-
Keeping that picture in mind helps match the right recovery tools to the right state.
The Neuroscience Of Burnout: How Chronic Stress Rewires Your Brain
Burnout is not a character flaw, lack of grit, or a mindset failure. It is what happens when the brain’s stress systems, meant for short emergencies, run at high volume for months or years. Those systems pull on hormones, neurotransmitters, and brain circuits in ways that can be measured on scans and in lab work.
The human stress response evolved to handle things like sudden threats and short‑term danger. Under those conditions, the brain floods the body with adrenaline and cortisol, increases heart rate and blood pressure, shifts blood flow to muscles, and sharpens focus on immediate threats. Once the danger passes, levels fall, and the system resets.
Modern stress often does not give that reset. Instead of short spikes, many people live with constant deadlines, alerts, financial worries, caregiving stress, and social pressure. The brain reads this as a never‑ending emergency. Over time, this pattern changes brain structure in regions that manage attention, memory, and emotional balance and keeps the fear center, the amygdala, on high alert. Understanding these changes helps explain why burnout feels so hard to think or willpower a way out of.
Structural Brain Changes In Burnout
Brain imaging research has compared the brains of people with chronic job burnout to those without it and found real structural differences. One key finding is less gray matter in parts of the frontal brain that help with emotional balance and complex thinking.
-
The anterior cingulate cortex (ACC) sits near the front of the brain and plays a big role in emotional regulation, empathy, and decision‑making under stress. When its gray matter volume drops, it becomes harder to manage strong feelings or keep perspective in tense situations. People may feel emotionally flooded by small triggers or, on the other side, numb and disconnected as a way to cope.
-
The dorsolateral prefrontal cortex (dlPFC) is another area that often shows changes in burnout. This region supports executive functions like planning, working memory, and flexible thinking. When it is not firing well, tasks that once felt easy, such as organizing a project or shifting between roles, suddenly feel draining and confusing. Simple decisions take longer, and multitasking becomes even more damaging.
Gray matter is made up mostly of neuron cell bodies—the parts of the brain that do the heavy processing. Losing volume in these areas is like having fewer or weaker processors to run complex programs. That is why someone in burnout can know what they should do but feel unable to execute the steps that used to feel automatic.
The Hyperactive Amygdala And Dysregulated Stress Response
Alongside these frontal changes, studies show an enlarged and hyperactive amygdala in many people with burnout. The amygdala is a small almond‑shaped structure deep inside the brain that helps detect threat and trigger the stress response.
Under normal conditions, the amygdala scans for danger, but the prefrontal cortex checks its work and keeps it from overreacting. In burnout, that braking system weakens. The amygdala fires more easily and more often, while the prefrontal cortex has less power to calm things down. The result is a nervous system that behaves as if danger is always present, even during quiet evenings at home or time off.
People feel this as constant tension, jumpiness, or a sense of impending doom. Even when they know on a logical level that an email or small delay is not life‑threatening, their body reacts with a racing heart, tight chest, and intrusive worry. This “wired but tired” state makes deep rest nearly impossible, which keeps the cycle going.
Allostatic Overload And The Cellular Cost Of Chronic Stress
Allostasis is the process by which the body maintains stability through change. When stress hits, the body adjusts to keep blood pressure, blood sugar, and temperature in safe ranges. Allostatic load is the wear and tear that builds up when those adjustments stay switched on too long.
Chronic stress keeps cortisol, adrenaline, and inflammatory signals elevated. This constant hormonal traffic is hard on blood vessels, immune cells, and, importantly, mitochondria. Firing the stress response is metabolically expensive; it burns through ATP and NAD+ at a rapid rate. Over months and years, this creates a cellular energy deficit where cells cannot keep up with repair and normal function.
That cellular drain is one reason burnout feels physical as well as emotional. Muscles ache, recovery lags, and the brain struggles with tasks that used to feel easy. It is also why recovery needs to happen on more than one level. Mindfulness, therapy, and boundaries help calm the stress response from the top down, while targeted support for mitochondria and NAD+ from approaches like Synchronicity Health’s NAD+ products helps rebuild from the bottom up.
Root Causes And Risk Factors: Who's Most Vulnerable To Burnout?

Burnout almost never comes from a single bad week or one stressful project. It tends to grow from a mix of work pressures, personal stress, lifestyle patterns, and social factors that, together, keep stress high and recovery low. Understanding those layers can help someone see why they feel the way they do and where their own leverage points might be.
Work is often the most visible arena for burnout, especially in high‑demand fields. Long hours, unclear expectations, and emotional labor all pile up. At the same time, home life can add caregiving, relationship tension, or financial worry to the load. Then modern technology keeps everything spinning by making people reachable every minute.
Some people are also more at risk because of personality, life role, or social position. Perfectionists, caregivers, women carrying invisible labor, and people facing discrimination all start out closer to the edge. Burnout, in that sense, is less about one person “not being strong enough” and more about the intersection between biology, psychology, and the environment they live in.
Workplace Stressors: Beyond Just Being Busy
Not all job stress is bad. Meaningful challenge can build skills and satisfaction. The problem comes when demands stay high while control, support, and recovery stay low. Certain patterns show up again and again in people who burn out:
-
Excessive workload: constant overtime, chronic understaffing, or roles that quietly stretch beyond the written job description.
-
Lack of control or autonomy: little say in how work is done, frequent changes without input, or heavy micromanagement.
-
Poor culture or values conflict: weak communication, unresolved conflict, or subtle punishment for setting boundaries. In some settings, people live with daily microaggressions or pressure to hide parts of who they are. When the values of the organization clash with personal ethics, or when hard work is rarely recognized, burnout risk climbs even for people who used to love their field.
Personal And Lifestyle Accelerants
Life outside of work can either buffer stress or pour gasoline on it. Even a fairly healthy job can feel unbearable when home life is chaotic or draining, and the reverse is also true.
Key accelerants include:
-
Caregiving responsibilities such as parenting young children, caring for aging parents, or supporting a partner with illness. The physical effort, sleep disruption, and emotional load add up, especially when support is thin or appreciation is low.
-
Relationship strain. Ongoing conflict at home erodes one of the main places people expect to recover.
-
Financial stress. Worrying constantly about bills, debt, or job security keeps the stress response running around the clock.
-
Health challenges in oneself or loved ones, which add demands on time, attention, and money.
-
Technology habits. Smartphones keep work messages, news, and social feeds a tap away. Remote work removes the physical line between office and home, often turning every room into potential workspace. Without firm boundaries, the brain never fully stands down.
-
Social isolation from busy schedules, relocation, or life stage, which removes one of the strongest buffers against stress: close, supportive relationships.
High-Risk Populations And Personality Traits
Certain traits and roles make burnout more likely even in the same environment. Recognizing these patterns is not about assigning blame; it is about spotting where extra protection is needed.
-
Perfectionists and high achievers often hold themselves to standards no one could maintain. They struggle to say things are “good enough,” take on extra work to avoid disappointing others, and ignore their own warning signs.
-
People‑pleasers tend to say yes to too many requests out of fear of conflict or rejection.
-
Women, especially women of color, report higher burnout rates. Many carry an extra layer of unpaid organizing and emotional labor at home while also facing bias or microaggressions at work.
-
Caregivers and helping professionals—including parents, adult children of ill parents, healthcare workers, educators, and emergency responders—often work under conditions of high need and low recognition.
-
Remote workers, freelancers, and expats can be at risk because of blurred boundaries and less built‑in social support.
For people in these groups, planning ahead for stress management, social support, and cellular recovery is not a luxury; it is a basic safety measure.
The Progression From Chronic Fatigue To Burnout: Recognizing The Warning Signs
Burnout rarely appears out of nowhere. It usually starts with understandable fatigue during a demanding season, then slowly shifts as the body and brain stop bouncing back. Because that slide is gradual, many driven people do not notice the line until they are far past it.
Early on, the story is often “just a busy quarter” or “this training cycle is intense, but it will calm down soon.” When the busy period ends, though, another one follows, or the person immediately fills freed‑up space with new goals. Over time, the nervous system never gets a true reset, and short‑term adaptations harden into long‑term patterns.
Seeing the stages helps a person act earlier. Instead of waiting for a full crash, they can notice when fatigue stops behaving like normal tiredness and start changing both their environment and their biology before structural changes in the brain and mitochondria get entrenched.
“If you don’t pick a day to rest, your body will pick it for you.” — Traditional saying
The Slippery Slope: When "Pushing Through" Backfires
The first stage is persistent fatigue that does not fully clear between stressors. Someone may notice they are tired most days even if they are sleeping seven or eight hours. Enthusiasm for work and training dips slightly, and irritability edges up. Yet because deadlines are real and goals matter, they tell themselves the tiredness is temporary.
Common thoughts in this phase sound like:
-
“I just need to get through this launch.”
-
“Once this project wraps, I will take a break.”
The problem arises when there is always another project or push phase. The nervous system learns that the promise of rest never arrives, so it holds stress hormones higher for longer.
As this continues, the second stage appears:
-
Coping tools that used to work start to fail.
-
People lean harder on caffeine, pre‑workout drinks, sugar, or late‑night scrolling to numb out, but sleep gets worse and mornings get harder.
-
Minor health issues—like frequent colds, headaches, or gut trouble—pop up more often.
Mentally, focus slips, and tasks that once felt exciting turn into chores. The story often shifts to “I just need to be more disciplined,” which drives more pushing and less recovery, deepening the trap.
The Tipping Point: From Adaptive To Maladaptive Stress Response
If nothing changes, the stress response crosses a tipping point. What started as an adaptive reaction to high demand becomes a source of damage in its own right. This is where chronic fatigue begins to morph into full burnout.
Signs of this shift include:
-
Exhaustion that feels baked in, not just present after a long day.
-
Energy that barely improves even after holidays or several nights of good sleep.
-
Emotional life shifting toward numbness or sharp reactivity.
-
Frequent thoughts like “What is the point?”
-
Work quality dropping despite increased effort, with more mistakes, forgetfulness, and missed details.
On a biological level, this stage reflects deepening brain and cellular changes. Stress circuits have been firing for so long that the amygdala–prefrontal balance is disrupted, and mitochondria have spent months oversupplying energy to that stress machinery. NAD+ levels often sit low, slowing ATP production and repair. At this point, simple stress management tips are not enough. Recovery needs targeted changes in workload, psychology, and cellular energy support.
Critical Warning Signs Requiring Immediate Action
Some signs mean it is time to stop wondering and start acting now. These are flags that the situation has moved beyond “normal busy life” into territory where health and safety are at risk.
Red flags include:
-
Persistent physical symptoms such as severe insomnia, chest pain, chronic digestive trouble, or pain that does not respond to normal care
-
Reliance on alcohol, nicotine, marijuana, or other drugs as the main way to relax, sleep, or get through the day
-
Thoughts of self‑harm, a sense that the future is blank, or a total inability to carry out basic tasks at work or home
If any of these show up, professional help is essential. As one psychiatrist put it, if substances have become the main coping tool, it is time to talk with someone. Early action does not just shorten recovery; it can prevent medical and psychological crises.
How To Fight Burnout: Comprehensive Recovery And Prevention Strategies
Once burnout is on the radar, the next step is building a recovery plan that is realistic and science‑based. Healing these patterns is less like flipping a switch and more like rehab after a major injury. Most people need several months of steady changes rather than one dramatic move.
The encouraging part is that the same strategies that help someone climb out of burnout also protect against future episodes. They work best when stacked: physical foundations, psychological tools, environmental changes, social support, and, when appropriate, targeted support for brain and cellular energy. For people who like clear frameworks, this section covers how to fight burnout day to day, while the next section focuses on how to fix burnout at the deeper cellular and neurological level.
The Non-Negotiable Foundations: Sleep, Nutrition, And Movement

Sleep is the foundation of every other recovery effort. During deep sleep, the brain clears metabolic waste, repairs synapses, and resets many stress signals. For burnout recovery, aiming for seven to nine high‑quality hours per night on a consistent schedule is a baseline, not a luxury. Simple steps such as dimming lights an hour before bed, keeping the bedroom cool and dark, and avoiding heavy meals late at night can make a big difference.
For people whose nervous systems feel stuck in high gear, targeted targeted sleep support can help break the pattern. Synchronicity Health offers melatonin and theanine nasal sprays designed to support faster sleep onset and deeper, calmer nights by directly influencing the nervous system through nasal delivery. These tools are not sedatives; they nudge the body toward the sleep it is already trying to have, which is especially helpful when stress hormones run high.
Nutrition is the next pillar. The brain and mitochondria run best on steady, whole‑food fuel rather than spikes of sugar and caffeine. Focusing meals around:
-
Protein
-
Fiber‑rich carbohydrates
-
Healthy fats
helps stabilize blood sugar and gives cells the raw materials they need to produce ATP and neurotransmitters. Relying on coffee, energy drinks, and sweets to push through the day may feel helpful in the moment but often leads to sharp dips in energy and mood later.
To support smoother metabolic control, many high performers add targeted metabolic support. Synchronicity Health’s Berberine with Ceylon Cinnamon is designed to support healthy glucose handling and insulin sensitivity, which in turn helps keep energy steadier across the day. When blood sugar swings are smaller, mitochondria can run ATP production more smoothly, and both physical and mental energy feel more even.
Movement is the third core element. Exercise helps regulate cortisol, increases brain‑derived neurotrophic factor (BDNF) that supports brain plasticity, and improves mitochondrial function. During burnout, the goal is not to chase personal records but to move consistently without overtaxing an already stressed system. Daily walks, light strength training, or yoga can provide the benefits of movement without adding more strain. For those ready to support exercise performance and cellular energy, Cordyceps mushroom products from Synchronicity Health can support oxygen use and endurance in a gentler way than stimulants.
Setting Boundaries And Managing Cognitive Load
Without boundaries, even perfect sleep and nutrition will not protect against burnout. The nervous system needs predictable off‑duty time to reset. This starts with simple but firm decisions, such as a set time each evening when work stops and devices stay closed. Protecting that time, even from “just one more email,” teaches the brain that rest is real.
Learning to say no is another key skill. Many burnout‑prone people take on extra projects, social commitments, or unpaid tasks out of habit. Practicing small refusals—turning down a nonessential meeting, delegating a task, or declining a social event when exhausted—builds the capacity to protect limited energy. For remote workers, creating a defined workspace and a physical “shutdown ritual,” like closing a laptop and leaving the room, helps separate work from home life.
Managing cognitive load is just as important as managing calendar time. The brain can only hold so much at once before performance drops. Working in 60–90 minute focus blocks, with short movement breaks in between, often yields better output than long, unfocused marathons. Single‑tasking—doing one meaningful task at a time—reduces the mental friction of constant task‑switching. External tools like task managers or written lists take pressure off working memory so the brain can focus on problem‑solving instead of remembering.
Digital boundaries help here as well:
-
Limiting nonessential notifications
-
Setting specific times to check email or social media
-
Scheduling “screen‑free” blocks
give the nervous system a break from constant stimulation. Short daily walks in nature, even in a city park, have been shown to lower stress markers and help the brain reset. For additional cognitive support, Synchronicity Health’s Clarity formulation combines fast‑acting ingredients with Lion’s Mane mushroom and other compounds aimed at long‑term brain health. It is designed for focused work without the jitters or crashes that come with heavy stimulant use.
How To Fix Burnout: Advanced Cellular And Neurological Interventions
For some people, addressing sleep, nutrition, movement, and boundaries is enough to reverse early burnout. For others—especially those who have been in a high‑stress state for years—the system needs deeper repair. This is where understanding and supporting cellular and neurological function becomes important.
Chronic stress draws heavily on mitochondrial energy and NAD+, reshapes brain circuits, and shifts hormones toward patterns that keep people stuck in “fight or flight.” Trying to fix that only with mindset work is like trying to run a high‑performance car on an empty tank. To create lasting change, it helps to work from both ends: calming the nervous system and restoring the cellular energy that supports normal brain function.
Synchronicity Health focuses on this deeper layer with physician‑designed products that aim at NAD+ biology, metabolic health, and stress resilience. For those asking how to fix burnout at the root, this combination of advanced supplementation with solid lifestyle change offers a practical path.
Rebuilding Cellular Energy: The NAD+ Foundation
NAD+ is central to energy metabolism. Every time mitochondria create ATP, NAD+ shifts electrons and cycles between oxidized and reduced forms. It also activates enzymes involved in DNA repair and cell survival pathways, including sirtuins that relate to aging and stress resistance. When NAD+ is low, all of these processes slow down.
By midlife, average NAD+ levels have dropped by around half compared with earlier adulthood. Chronic psychological stress, intense physical training without enough recovery, and poor sleep can drain it further. When this happens, cells struggle to meet energy demand, repair daily damage, and keep stress signaling in check. The lived experience is persistent fatigue, brain fog, slower recovery from workouts, and a general sense that “the battery never charges to 100%.”
Restoring healthy NAD+ availability is therefore a powerful base move for burnout recovery. Supporting NAD+ helps mitochondria increase ATP output, boosts DNA repair activity, and supports cellular stress responses. This is not about quick stimulation; it is about giving the hardware the molecules it needs to run well again.
Synchronicity Health approaches this with NAD+ nasal sprays and NMN products. Nasal delivery bypasses much of the digestive tract and uses the rich blood supply and proximity to the brain to provide fast, efficient support. NMN (nicotinamide mononucleotide) acts as a direct precursor that cells can convert into NAD+. These products are designed by a Yale‑trained physician and are third‑party tested for purity, potency, and contaminants, which matters for people who care about lab‑level quality.
Compared with IV NAD+ clinics that can cost hundreds or thousands of dollars per course, nasal sprays and oral precursors offer a more accessible way to support the same pathway at home. Many users report better daytime energy, clearer thinking, and improved workout recovery over two to three weeks of consistent use as NAD+ pools rebuild. The key is consistency and pairing NAD+ support with the foundational sleep and nutrition steps covered earlier.
Supporting Stress Resilience And Nervous System Regulation
Fixing burnout also means helping the nervous system come out of chronic high alert. Alongside therapy and behavioral tools, certain nutrients and plant compounds can support calmer, more adaptive stress responses.
-
Adaptogenic mushrooms are one helpful group. Reishi has a long history of use for calming, immune balance, and sleep support. Cordyceps supports oxygen use and may help with physical stamina and feelings of fatigue. Lion’s Mane supports nerve health and has been studied for its ability to increase BDNF, which helps the brain build and repair connections. Synchronicity Health’s Forage blend brings these mushrooms together to support whole‑system resilience rather than just chasing one symptom.
-
Cortisol balance is another key target. In burnout, cortisol can be chronically high, flat, or otherwise out of rhythm. Phosphatidylserine is a nutrient that has been shown to help lower excessive cortisol responses and support more normal patterns. Many people notice easier sleep onset, fewer “wired at midnight” nights, and a calmer body when dealing with daily stress.
-
Mood and relaxation also matter. Kanna, a South African plant, influences serotonin systems and has been used for mood and stress support. Synchronicity Health’s Kanna nasal spray is designed for relatively fast effects through nasal delivery, making it a useful tool during acute stress spikes or when shifting from work mode into rest mode. Used as part of a broader routine, it can help ease the emotional edge while deeper repairs take place.
Synchronicity Health’s Sync Stack concept ties these elements together. A typical burnout‑focused stack might include:
-
NAD+ and Clarity in the morning for cellular energy and focused work
-
Forage mushrooms during the day for resilience
-
A mix of sleep support and phosphatidylserine in the evening to calm the nervous system
These are meant to work alongside, not instead of, lifestyle and therapeutic work.
Metabolic Health And Blood Sugar Stability
Metabolic health underpins both physical and mental energy. Even without diabetes, frequent swings in blood sugar can create cycles of high energy followed by crashes, cravings, and irritability. The brain depends heavily on steady glucose supply; when levels spike and crash, focus and mood often follow the same pattern.
Supporting better glucose handling smooths out these swings. Synchronicity Health’s Berberine with Ceylon Cinnamon is designed to support insulin sensitivity and healthy blood sugar management. When glucose enters cells more efficiently, mitochondria receive a steadier fuel stream, ATP production is more consistent, and energy feels less like a roller coaster. This is especially helpful for people who notice mid‑afternoon crashes or intense sugar cravings when stressed.
Vitamin B12 is another part of the metabolic picture. It is necessary for red blood cell formation and energy metabolism in the nervous system. Low B12 can mimic or worsen fatigue, brain fog, and mood symptoms. Including adequate B12 intake—through diet and supplementation when needed—is part of any serious burnout recovery plan.
Building Long-Term Resilience: Lifestyle And Mindset Shifts
Once the worst of burnout passes, the next step is building a life that does not push the system back into the same corner. Resilience here does not mean never feeling stressed again; it means having structures, habits, and internal skills that let stress rise and fall without turning into chronic overload.
Long‑term protection comes from aligning daily rhythms with biology, matching goals with values, and strengthening social connections. Supplements and protocols from Synchronicity Health fit into this as ongoing support for energy and brain health, but they work best in the context of a life that is not constantly fighting basic physiological patterns.
Aligning With Your Circadian Rhythm
Many people with burnout describe feeling exhausted even when basic lab tests look normal. In a large number of those cases, the issue is less about a classic disease and more about circadian rhythm disruption. The internal clock that coordinates sleep, hormone release, digestion, and temperature has fallen out of sync with the outside world.
Artificial light at night, irregular sleep and meal times, shift work, and constant screen exposure all nudge that clock off track. Once the rhythm is disturbed, people may feel wired late at night and sluggish in the morning, hungry at odd times, or mentally foggy during normal work hours. Realigning the circadian system is one of the most powerful, low‑cost steps a person can take.
Helpful strategies include:
-
Getting bright natural light within an hour of waking to anchor the morning phase
-
Keeping evenings dim with warmer light, fewer screens, and a calm routine to signal the brain to prepare for sleep
-
Keeping sleep and wake times similar even on weekends to train the clock to be reliable
-
Eating most calories in a daytime window rather than late at night to support both circadian timing and metabolic health
-
Exercising earlier in the day, which usually fits better with natural cortisol curves
Synchronicity Health designs its product timing with these rhythms in mind. Cognitive and NAD+ support make the most sense earlier in the day, when focus and energy demands peak. Sleep and relaxation and relaxation support work best in the evening, when the goal is to help the nervous system shift into repair mode. Putting supplements on top of rhythm‑aligned habits amplifies their impact.
Re-Evaluating Goals, Values, And Priorities
Burnout is often a sign that the way a person is living does not match what matters most to them. Once the fog starts to lift, it can be a powerful time to reassess goals and values so that future effort goes where it truly counts.
A practical starting point is to:
-
List the top five personal values—things like health, family, creativity, service, freedom, or mastery.
-
Compare that list to where time and energy actually go in a normal week.
Many people discover that most of their hours are going into areas that do not rank high in their values, while the things they say matter most get the scraps.
From there, changes can be made piece by piece:
-
Career reassessment might mean setting new boundaries in a current job, shifting roles within an organization, or planning a longer‑term transition to work that fits better.
-
Relationship inventories can highlight which connections feel nourishing and which ones drain energy without giving much back.
-
Obligation audits help identify committees, clubs, or favors that once made sense but no longer do.
Developing healthier coping patterns is part of this shift. Instead of escaping from stress only through binge‑watching, endless scrolling, or substances, approach‑oriented strategies focus on either changing the stressor or changing the response. Problem‑focused tools might include direct conversations, renegotiating responsibilities, or seeking help. Emotion‑focused tools include mindfulness, reframing, journaling, breathwork, and creative outlets. Having several options ready makes it more likely that the next rough season does not slide into burnout again.
The Power Of Social Connection
Humans are wired for connection, and social ties are one of the strongest protective factors against burnout. Isolation, on the other hand, amplifies stress and makes it easier for hopeless thoughts to take hold. Burnout grows in silence and shame; it loosens when people share what is happening and receive real support.
Rebuilding or deepening connection can start small. It might mean:
-
Telling a close friend or partner honestly how exhausted and stuck things feel, instead of pretending everything is fine
-
Scheduling regular face‑to‑face time—coffee, walks, shared workouts—with people who feel safe and supportive
-
Joining a group with shared interests, whether fitness‑related, creative, or professional
Professional connection counts as well. Therapists, coaches, and support groups focused on stress and burnout provide spaces where these experiences are normal to talk about. One psychiatrist’s advice is simple: ask for help, period. That step alone often marks the turning point from silent struggle to active repair.
When To Seek Professional Help: Therapy, Coaching, And Medical Intervention
Self‑directed changes can carry a person a long way, especially in early stages of fatigue and overwhelm. There comes a point, though, where going it alone stops working. At that point, bringing in professionals is not a sign of failure; it is a smart way to shorten suffering and prevent more serious health problems.
Professional help can come from several directions: mental health providers, medical clinicians, and specialized coaches. Each plays a different role, and many people benefit from a team approach over time. The key is knowing when self‑care needs to be backed up by outside support.
Recognizing When Self-Help Isn't Enough
Certain patterns suggest it is time to bring in a professional rather than trying another solo tweak. One major sign is persistence. If someone has been improving sleep, nutrition, movement, and boundaries for several weeks and still feels deeply exhausted, hopeless, or numb, extra help is wise. When functioning at work or home drops to the point that basic duties are missed regularly, support becomes even more important.
Another signal is physical health. Chronic pain, frequent infections, severe insomnia, or other ongoing symptoms under stress warrant a medical evaluation to rule out or address conditions such as thyroid problems, anemia, autoimmune issues, or sleep disorders. Mental and physical health often dance together; ignoring one side makes it harder to heal the other.
Substance use is another clear marker. When alcohol, nicotine, marijuana, or other drugs become the main way to cope with stress or sleep, risk rises sharply. Thoughts of self‑harm, a sense that there is no future, or feeling emotionally flat most of the time are also reasons to seek care immediately. Clinicians often say that earlier intervention shortens recovery and reduces the chance that brain and body changes from burnout become deeply entrenched.
Types Of Professional Support
Different professionals address different aspects of burnout, and many people benefit from combining them over time.
-
Psychotherapy (talk therapy) is often a central piece. Therapists help people understand how they reached their current state, process difficult experiences, spot unhelpful thought patterns, and build new coping skills. Approaches like Cognitive Behavioral Therapy (CBT) focus on the connection between thoughts, feelings, and behaviors, while other methods focus more on past experiences, acceptance, or body‑based techniques.
-
Medical providers also have a role. Primary care clinicians can check for medical contributors to fatigue and burnout symptoms, such as nutrient deficiencies, hormonal issues, infections, or sleep apnea. Psychiatrists can evaluate for depression, anxiety, or other conditions that often overlap with burnout and, when appropriate, may prescribe medication to help stabilize mood, sleep, or anxiety so that therapy and lifestyle changes are easier to do.
-
Burnout‑focused coaches and counselors sit at the intersection of psychology and practical life design. They work on time management, boundary setting, communication, and career or role adjustments. While they do not replace therapy or medical care, they can be very helpful for turning insights into daily habits.
Throughout this process, advanced support for cellular and brain health—such as NAD+ products, metabolic support, and adaptogenic stacks from Synchronicity Health—can complement professional care. Many clinicians are open to integrating these tools into a broader plan, especially when products are physician‑designed and third‑party tested. The shared goal is the same: to restore energy, clarity, and a sustainable way of living.
Conclusion
Differentiating fatigue vs burnout is more than a language game. It shapes whether someone takes a long weekend and moves on or steps back and rebuilds their life and biology from the ground up. Fatigue is the body’s signal that recent demands have exceeded recovery but can usually be balanced with sleep, food, and smart rest. Burnout is the deeper state where stress has rewired brain circuits, drained cellular energy, and eroded motivation and meaning.
The path out begins with honest assessment: noticing how rest affects energy, watching for emotional numbness or deep hopelessness, and spotting the slide from “I am tired” toward “Nothing I do matters.” From there, foundations like sleep, nutrition, gentle movement, boundaries, and social support provide the base. Therapy, medical care, and skilled coaching add structure and expertise when self‑help is not enough.
For those who care about high performance and long‑term health, attending to the cellular side of this story is equally important. Supporting NAD+, mitochondrial function, and metabolic health through carefully designed products such as the nasal sprays, mushroom blends, and Sync Stacks from Synchronicity Health helps restore the energy systems that chronic stress has drained. When those biological repairs line up with sustainable habits and aligned priorities, the nervous system can move out of survival mode and back into a state where work, training, and relationships feel challenging in satisfying ways, not crushing ones.
FAQs
What is the biggest difference between fatigue and burnout?
Fatigue is a temporary state usually linked to a clear cause, such as intense training, late nights, or a busy week. It tends to improve with several days of better sleep, nutrition, and lighter demands. Burnout is a long‑lasting state where exhaustion, cynicism, and low effectiveness persist even after rest. People with burnout often feel emotionally numb or hopeless and struggle to imagine feeling better without major changes.
How can I tell if I am just overwhelmed or actually burned out?
Overwhelm feels like having far too much to do and not enough time, while still caring deeply about outcomes. There is a lot of stress and anxiety, but also strong engagement. Burnout usually includes emotional distance, a sense that nothing matters, and a drop in motivation even for things that used to be meaningful. If good sleep and a lighter schedule restore your energy and engagement, overwhelm is more likely. If dread and emptiness return quickly after rest, burnout is more likely.
Can supplements alone fix burnout?
Supplements can play an important supporting role, especially those that target NAD+, mitochondrial function, metabolic stability, and nervous system balance. They can help restore the physical capacity for energy and focus. However, burnout almost always has psychological and environmental roots as well. Without changes in workload, boundaries, coping skills, and sometimes therapy or medical care, supplements on their own are unlikely to resolve the problem fully.
When should I consider products from Synchronicity Health?
Synchronicity Health products make the most sense for people who are already working on sleep, nutrition, movement, and boundaries but still feel a gap in energy, focus, or recovery. If you suspect that chronic stress has drained your cellular energy—showing up as stubborn fatigue, brain fog, and slow recovery—then NAD+ nasal sprays, NMN, metabolic support, and adaptogenic stacks can be valuable additions. When in doubt, discussing these options with a healthcare provider who understands both burnout and cellular health is a wise next step.




Leave a comment
All comments are moderated before being published.
This site is protected by hCaptcha and the hCaptcha Privacy Policy and Terms of Service apply.